
Colonoscopy is a diagnostic technique that allows physicians to visually inspect the interior lining of the colon. Colonoscopy is performed by a physician specially trained in the procedure and is commonly used as a screening tool for colon cancer. The exam is performed with an instrument called a colonoscope, which is inserted into the rectum and through the colon. When screening for colon cancer, the physician is looking for polyps and other abnormal lesions. 1 The United States Preventive Services Task Force (USPSTF) recommends that adults aged 45 and older get screened for colon and rectal cancer by colonoscopy.2
The following sections describe colonoscopy in more detail:
- Colonoscopy Instruments
- What to Expect During a Colonoscopy
- Preparation for a Colonoscopy
- The Colonoscopy Exam
- Colonoscopy Results
- Disadvantages of Colonoscopies
- Virtual Colonoscopy
- Colonoscopy vs Virtual Colonoscopy
Colonoscopy Instruments
The instrument used during a colonoscopy is known as a colonoscope. It is a long, flexible tube that is inserted through the rectum. The colonoscope has a light source and a tiny video camera that allows physicians to view the inside of the colon on a video screen. The physician is also able to take pictures of unusual lesions or record the entire process, providing a lasting record of the exam that may be reviewed if necessary.1
The colonoscope tube contains a channel through which the physician is able to pump air into the colon to inflate it, this allows for a better visualization of the inside lining. The physician can also insert instruments into the colon through the channel to take tissue samples, remove polyps, inject solutions, or burn (cauterize) tissue. For example, if a polyp is identified in the colon a wire loop known as a "snare" will be sent through the tube and used to remove the polyp, this process is called polypectomy. In some cases, a mild electric current will be sent through the tube to cauterize the tissue to prevent bleeding.1
What to Expect
Before the Exam
Before the examination the patient will change into a gown and will receive an injection to minimize discomfort. This medicine may make the patient drowsy for several hours. Before the procedure begins, the patient will most likely have to sign a permission form that states that they understand what the test involves. NOTE: If a patient is regularly taking narcotic painkillers such as Percodan®, Percocet®, or codeine, they should inform the anesthesiologist.3
How it Feels
Although colonoscopy is relatively painless, it can be uncomfortable. Patients may be given mild sedatives to help them relax. As the colonoscope is inserted into the colon, air is pushed into the patient through the tube, so the patient may feel the need to defecate. This feeling is normal, but if it persists, the physician should be informed so that more medication can be administered to the patient to help them relax.1
After the Exam
After the exam, the patient will be positioned on his or her left side on the colonoscopy table, which is comfortably padded. A small oximeter probe will be placed on the patient's fingertip to monitor pulse rate and breathing function during the exam if anesthesia was used. The probe is not invasive and does not cause any pain. In some cases, a narrow oxygen tube may be used to provide small amounts of oxygen to the patient.
Preparation
In order for a colonoscopy to be effective and accurate, the colon must be extremely clean so that the colonoscope can navigate through without being blocked by stool. There must not be any solids or liquids present that could obscure the view of the camera. What a patient does the days preceding the exam can directly affect how well the colon can be examined. To prepare for the procedure, most patients will be asked to do the following:
- Discontinue use of iron pills or other medications containing iron because iron can change the color of the colon lining.
- Take laxatives and enemas that are prescribed by their doctors. The bowel movements caused by these treatments clear the bowel and make the imaging process easier.
- While drinking the laxative, take a 5 minute walk every 10 minutes
- Avoid eating solid foods and opaque liquids
- Drink only clear liquids such as black coffee, tea, water, clear broth, and juices without pulp. Eat only soft foods such as JELL-O®, but nothing that is red in color, since it can affect the colon lining.
On the day of the exam, the patient may be asked to not eat at all, or restricted to a diet of only clear, non-alcoholic liquids. Patients who have diabetes or are taking blood thinners may have different guidelines that they should follow and should consult their physicians for specific instructions about pre-exam preparation.
In rare cases, the phosphate-based laxative has caused kidney damage in healthy older adults, people taking medication for hypertension, arteriosclerosis, or heart disease, and those with chronic kidney disease. Patients who are in one of these categories may be given a special type of cleansing solution.1
Patients should wear loose, comfortable, casual clothing that can be easily removed because most likely, a gown will be provided. Patients should also leave their jewelry and valuables at home.
The Exam
Procedure
After the patient is prepared, the doctor will lubricate the rectal opening, insert the colonoscope and guide it through the length of the colon. The doctor will look closely at the colon walls searching for any abnormality. During the procedure air may be pumped through the colonoscope to inflate the colon, this makes it easier for the doctor to see all the nooks and crannies. The air may cause a feeling of abdominal fullness, but should not cause pain. Abdominal cramping and pressure is normal during this procedure. As the colonoscope travels further into the colon, the patient may be asked to shift their position to help guide the tube through the colon.4, 5
In some cases the entire colon is not able to be examined. This may be caused by the following:
- inadequate bowel preparation
- patient discomfort and/or intolerance
- extra colon tissue blocking the path
- scarring from past abdominal surgeries
- severe diverticular disease
If a colonoscopy is unsuccessful in viewing the entire colon, another procedure may be required. Possible options include repeat colonoscopy, double-contrast barium enema, computed tomography colonography (CTC), and colon capsule. This decision depends on various factors, such as the indication for the original colonoscopy, patient characteristics, and available technologies.3
Recovery
The procedure usually lasts between 20-60 minutes. Colonoscopies are outpatient procedures in most cases, so patients may go home after the procedure is complete. However, if the patient was sedated during the test a ride home should be arranged. The patient should rest and relax for the rest of the day until the effects of the medication are gone. After colonoscopy, it's normal to feel bloated or to pass gas for a few hours, walking may help ease the unpleasant feeling. A small amount of blood may appear in first bowel movement following the exam, this is normal. However, if the patient repeatedly passes blood, has recurrent abdominal pain, or a fever of 100°F or higher, they should seek medical attention. It is also important to alert the doctor if severe abdominal swelling (distension) occurs after a colonoscopy.1
Colonoscopy Results
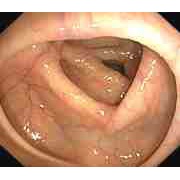
Normal Colon
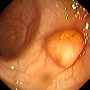
Colon with Polyp
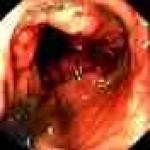
Colon Cancer
Images from Gastrolab.
A colonoscopy allows a doctor to examine the inside of the entire colon for abnormalities, including; intestinal inflammation, ulceration, bleeding, diverticulitis, colitis, colon polyps, and tumors. Negative - the doctor finds nothing unusual. The patient may not need to get another colonoscopy for several years. Positive - the doctor finds something suspicious of disease. The patient needs to undergo more frequent screenings. If a few small polyps (1 cm or less) are found, the patient may not need a colonoscopy for another 5-10 years, depending on other risk factors. If many, large polyps or polyps with pre-cancerous cells are found the patient may be advised to get a colonoscopy every 3-5 years. Biopsy After Colonoscopy If an abnormality is seen, the doctor may decide to remove it or take a tissue sample (biopsy) for analysis. A specially trained doctor called a pathologist will examine the tissue with a microscope and determine the diagnosis. A biopsy can help determine the nature of the tissue (benign or cancerous) and help the physician decide whether the abnormality needs to be removed. To obtain a biopsy, metal forceps are passed through the scope and used to snip off a portion of colon tissue. Alternatively, the doctor may decide to take a brushing of the colon lining to evaluate an area of suspected abnormality. In this case, a small nylon brush is passed through the center of the colonoscope and is rubbed against the colon lining to retrieve a small tissue sample. Regardless of which procedure is performed, the patient will feel no pain or sensation. Remember: just because the doctor decides to take a biopsy, this does not necessarily mean cancer is suspected. Biopsies can also help diagnose other problems such as inflammation and ulcers. If tissue is removed during a colonoscopy, a follow-up meeting may be scheduled to allow the patient and physician to discuss the results.
Possible Disadvantages
Colonoscopy is an effective way to view the colon, but there are disadvantages to this exam:
Ineffective Exam
Sometimes a colonoscopy is not effective in examining the entire colon. If the colon is not clean or there is a blockage the doctor may not be able to examine the entire colon. This may cause abnormalities to be missed. A barium enema or virtual colonoscopy may also be required in these cases. An older study, from 1997, showed that colonoscopy failed to examine the entire colon in 10-15% of cases and missed 10-20% of lesions.6
Possible Side Effects
In most cases colonoscopy doesn't produce any side effects, but they can occur.
- For some patients colonscopy is uncomfortable, painful, and may cause anxiety. These patients can be given some form of sedative/anesthetic to reduce those feelings. Whenever a sedative/anesthetic is used there is a risk for side effects, including drowsiness, nausea, and/or pain at the site of injection.
- Damage to the colon can occur from colonoscopy or colon biopsy. A study from 1997 showed tearing of the colon lining occurred in one out of every 500-1000 cases.6
- Colonoscopies can be expensive (from $500-$1000), three times more expensive than a barium enema. Check with your insurance provider about coverage for this test.
Virtual Colonoscopy
Virtual colonoscopy is another screening technique for colon cancer. Unlike the conventional colonoscopy, virtual colonoscopy uses a computed tomography (CT) scanner and computer graphics to create 3D images of the colon. A radiologist analyzes the images to detect abnormalities.
Advantages
Virtual colonoscopy is more comfortable for the patient than conventional colonoscopy because it does not require sedation and does not involve inserting a colonoscope into the rectum. It also takes less time for a virtual colonoscopy (only between 15-20 minutes) and has the ability to screen organs surrounding the colon for abnormalities.
Disadvantages
Virtual colonoscopy does have some disadvantages compared to conventional colonoscopy. The doctor cannot remove polyps or take tissue samples from suspicious areas, if a lesion is detected an conventional colonoscopy may be needed to further investigate the abnormality. Also, an virtual colonoscopy is unable to provide information about mucosal detail and color, which is useful in the characterization of lesions.
Like all detection methods, virtual colonoscopy is not 100% effective in detecting disease.7, 8
Preparation for a Virtual Colonoscopy
Preparation
The preparation is simlar to that of a traditional colonoscopy. Before the exam patients must remove any stool from the colon. Also, an oral contrasting agent is taken the day before the examination to increase image quality.
Virtual Colonoscopy Procedure
A small enema tip is inserted into the patient's rectum to introduce air into the colon; this is the only invasive part of the exam. The rest of the exam consists of a series of x-rays that are taken while the patient is positioned comfortably on their back and stomach.9, 10
Other than the temporarily feeling of abdominal cramping or gas pains from the air inserted into colon, the exam is easy and painless. The exam is also quick and because no anesthesia is needed the patient can resume normal activities immediately after a virtual colonoscopy. Colon perforation is not a risk because the exam is non-invasive.9, 10
Conventional vs Virtual Colonoscopy
A 2003 study compared the performance of CT virtual colonoscopy with conventional optical colonoscopy in 1233 asymptomatic adults (mean age 57.8). The results are summarized below:
Polyp diameter 6 mm or more:
- Polyp diameter 10 mm or more:
- Conventional Colonoscopy: 87.5% sensitivity
- Virtual Colonoscopy: 93.8% sensitivity
- Polyp diameter 8 mm or more:
- Conventional Colonoscopy: 91.5% sensitivity
- Virtual Colonoscopy: 93.9% sensitivity
- Conventional Colonoscopy: 92.3% sensitivity
- Virtual Colonoscopy: 88.7% sensitivity
The specificity of virtual colonoscopy was 96% for polyps at least 10mm in diameter, 92.2% for polyps at least 8mm in diameter, and 79.6% for polyps at least 6mm in diameter. Two of the polyps detected were malignant, both of which were detected by virtual colonoscopy. However, one of these was missed by optical colonoscopy.11
The researchers concluded that CT virtual colonoscopy is a useful, accurate method for screening of colorectal cancer in average-risk adults. Research is still being conducted to evaluate the utility of this technique in colon cancer screening.12, 13
- 1abcdef JD Waye. "Colonoscopy". CA: A Cancer Journal for Clinicians. 1992;42(6):350-65. [PUBMED]
- 2 Force, U., Davidson, K., Barry, M., Mangione, C., Cabana, M., Caughey, A., … Wong, J. (2021). Screening for Colorectal Cancer: US Preventive Services Task Force Recommendation Statement. JAMA, 325(19), 1965–1977. http://doi.org/10.1001/jama.2021.6238 (Original work published December 2021) [PUBMED]
- 3ab Franco, D., Leighton, J., & Gurudu, S. (2017). Approach to Incomplete Colonoscopy: New Techniques and Technologies. Gastroenterology & Hepatology, 13(8), 476–483. (Original work published August 2017) [PUBMED]
- 4 Seward, E. (2019). Recent advances in colonoscopy. F1000Research, 8. http://doi.org/10.12688/f1000research.18503.1 (Original work published December 2019) [PUBMED]
- 5 Lee, S.-H., Park, Y.-K., Lee, D.-J., & Kim, K.-M. (2014). Colonoscopy procedural skills and training for new beginners. World Journal of Gastroenterology, 20(45), 16984–95. http://doi.org/10.3748/wjg.v20.i45.16984 (Original work published December 2014) [PUBMED]
- 6ab Fenlon, HM and Ferrucci, JT. "Virtual Colonoscopy: What Will the Issues Be?." American Journal of Roentegenology. 1997 Aug;169(2):453-8. [PUBMED]
- 7 Pinkhardt PJ, Kim DH. (2008) Computerized tomography colonography: a primer for gastroenterologists. Clin Gastroenterol Hepatol. May;6(5):497-502. [PUBMED]
- 8 Kim DH, Pickhardt PJ, Hanson ME, Hinshaw JL. (2010) CT colonography: performance and program outcome measures in an older screening population. Radiology. Feb;254(2):493-500. [PUBMED]
- 9ab "Virtual Endoscopy." Radiology Regional Center. [Virtual Colonoscopy Guide]
- 10ab "Virtual Colonoscopy." The Center for Virtual Colonoscopy at Boston Medical Center. [http://www.virtualcolonoscopy.net/]
- 11 Pickhardt PJ, et al. "Computed Tomographic Virtual Colonoscopy to Screen for Colorectal Neoplasia in Asymptomatic Adults." N Engl J Med. 2003 Dec 4;349(23):2191-200. Epub 2003 Dec 1. [PUBMED]
- 12 Lin, OS. 2010. Computed tomographic colonography: hope or hype? World J Gastroenterol. Feb 28;16(8):915-20. [PUBMED]
- 13 LaBundy J, Prather CM. Choices in colorectal cancer screening: a review of current screening modalities and recommendations. Mo Med. 2009. Sep-Oct;106(5):351-5. [PUBMED]
